Onychomycosis is an infection of the nail caused by fungi such as dermatophytes, non-dermatophyte moulds and yeasts (mainly Candida species). Of these 80% of the toenail infections are caused by dermatophytes (Trichophyton rubrum). Onychomycosis is classified clinically as distal and lateral subungual onychomycosis (DLSO), superficial white onychomycosis (SWO), proximal subungual onychomycosis (PSO), candidial onychomycosis and total dystrophic onychomycosis.
Distal and lateral subungual onychomycosis:
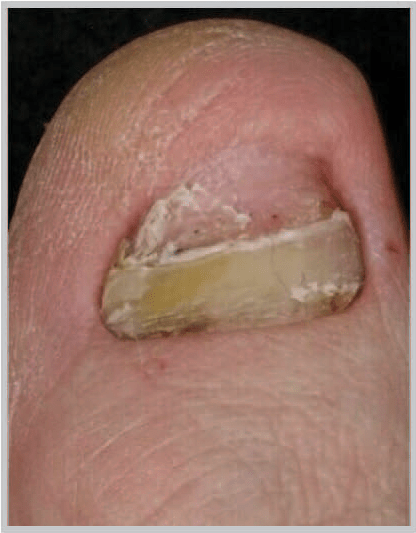
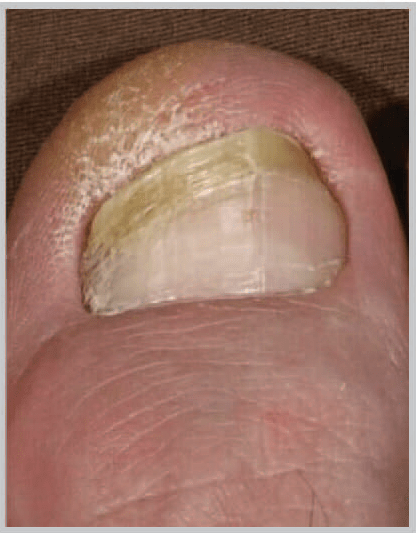
Distal and lateral subungual onychomycosis are seen in majority of cases and is almost always due to dermatophyte infection. It affects the hyponychium, often at the lateral edges initially, and spreads proximally along the nail bed resulting in subungual hyperkeratosis and onycholysis although the nail plate is not initially affected. Distal and lateral subungual onychomycosis may be confined to one side of the nail or spread sideways to involve the whole of the nail bed, and progresses relentlessly until it reaches the posterior nail fold. Eventually the nail plate becomes friable and may break up, often due to trauma, although nail destruction may be related to invasion of the plate by dermatophytes that have keratolytic properties. Examination of the surrounding skin will nearly always reveal evidence of tinea pedis. Toenail infection is an almost inevitable precursor of fingernail dermatophytosis, which has a similar clinical appearance although nail thickening is not as common
Superficial white onychomycosis:
Superficial white onychomycosis is also, also a dermatophyte infection, which is caused by T. mentagrophytes. It is much less common than distal and lateral subungual onychomycosis and affects the surface of the nail plate rather than the nail bed. Discoloration is white rather than cream and the surface of the nail plate is noticeably flaky. Onycholysis is not a common feature of superficial white onychomycosis and intercurrent foot infection is not as frequent as in distal and lateral subungual onychomycosis.
Proximal subungual onychomycosis:
Proximal subungual onychomycosis is an uncommon variety of dermatophyte infection often related to intercurrent disease. Immunosuppressed patients, notably those who are human immunodeficiency virus-positive, may have a variety of dermatophyte infection; conditions such as peripheral vascular disease and diabetes also may present in this way. Evidence of intercurrent disease should therefore be considered in a patient with proximal subungual onychomycosis.
Candidal onychomycosis:
Infection of the nail with Candida yeasts may present in one of the following four ways, (i) chronic paronychia with secondary nail dystrophy; (ii) distal nail infection; (iii) chronic mucocutaneous candidiasis; and (iv) secondary candidiasis.
Chronic paronychia of the fingernails generally occurs in patients with wet occupations. Swelling of the posterior nail fold occurs secondary to chronic immersion in water or possibly due to allergic reactions to some foods, and the cuticle becomes detached from the nail plate thus losing its water-tight properties. Microorganisms, both yeasts and bacteria, enter the subcuticular space causing further swelling of the posterior nail fold. Distal nail infection with Candida yeasts is uncommon and virtually all patients have Raynaud’s phenomenon or some other form of vascular insufficiency.
Chronic mucocutaneous candidiasis, involves the mucous membranes which is caused due to diminished cell-mediated immunity. Clinical signs vary with the severity of immunosuppression, but in more severe cases gross thickening of the nails occurs, amounting to a Candida granuloma. Secondary candidal onychomycosis occurs due to other diseases of the nail, mostly psoriasis
DIAGNOSIS
Fifty percent of all nail dystrophy are fungal in origin; it is not always possible to identify such cases accurately. Treatment period of the nail are mostly long-term and it takes time for the nail to grow completely before the treatment can be rendered as successful. Laboratory diagnosis consists of microscopy to visualize fungal elements in the nail sample and culture to identify the species concerned. The success of such tests depends upon the quality of the sample, the experience of the microbiologist and the ability of the laboratory to discriminate between organisms that are likely pathogens, organisms growing in the nail as saprophytes, and contamination of the culture plate. The addition of Parker’s blue or black ink may enhance visualization of the sample
Why is the treatment necessary?
Onychomycosis, leads to discoloration and deformation of the nails. Particular problems include thickening, which may cause pain and make basic nail cutting difficult. In patients with complicating factors, deformed nails can lead to surrounding tissue damage and once again promote secondary bacterial infection. Furthermore, a recent study has highlighted the psychological, social and occupational effects of the condition which appear to have been underestimated by health care professionals for treating the condition.
Treatments For Onychomycosis:
A. Laser Treatment
B. Oral Anti-fungal Treatment
Laser Treatment:
With the help of a Laser, heat energy is used to kill the fungal elements. Compliance is very important in this procedure. The patient will be coming in on weekly basis for 6-8 wks and then based on the improvement, the touch-ups will be required.
Oral Anti-Fungal Treatment:
Routine blood work will be needed until the continuation of the medication
PRECAUTIONS:
While the onchomycosis treatment is in process, all the old socks need to be replaced with new socks and any shoes which were worn without socks should not be used. Since the risk of reinfection is very high, all the safety precautions need to be taken accordingly.
Welcome to Zaytuna Medical Spa, where taking care of your skin is our only priority. Located in the prestigious intersection of peel, Vaughan, Toronto, and Peel regions. we offer high-end skin treatments in a clean and cozy atmosphere. We take pride in creating highly customized treatments that are as unique as you. Our services include Medical-grade Facials, Photo Facial, Laser Hair Removal, Botox, Fillers, PRP, Hair Restoration Therapies, Microneedling, and Chemical Peel. Our professional, friendly team is ready to assist you with the most luxurious treatments in skincare.
As a highly experienced Physician at Zaytuna Medical Spa, Dr.Sabha Cheema believes that healthy, glowing skin begins with exceptional care. Her experience proves that anyone can achieve healthy skin through proper advice, care, and customized treatments for your skin.
